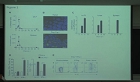
Evidence has emerged that intestinal dysbiosis is associated with diverse pathological processes, including diabetes, obesity, and inflammatory bowel disease. In this study, we demonstrated intestinal barrier disruption and aberrant mucosal immunity i...
http://chineseinput.net/에서 pinyin(병음)방식으로 중국어를 변환할 수 있습니다.
변환된 중국어를 복사하여 사용하시면 됩니다.
- 中文 을 입력하시려면 zhongwen을 입력하시고 space를누르시면됩니다.
- 北京 을 입력하시려면 beijing을 입력하시고 space를 누르시면 됩니다.
Intestinal barrier disruption and dysregulated mucosal immunity contribute to kidney fibrosis in CKD
한글로보기부가정보
다국어 초록 (Multilingual Abstract)
Evidence has emerged that intestinal dysbiosis is associated with diverse pathological processes, including diabetes, obesity, and inflammatory bowel disease. In this study, we demonstrated intestinal barrier disruption and aberrant mucosal immunity in 5/6 nephrectomized mice and the effect of probiotics on these parameters, systemic inflammation, and the progression of CKD. In CKD mice, the expression of colon HSP 70, a key protein in intestinal barrier integrity, and tight junction protein claudin-1 was significantly decreased; however, pore-forming claudin-2 expression and the incidence of apoptosis in colon epithelial cells was increased. These changes were accompanied by increased permeability. Although the percentage of CD4+ Foxp3+ Tregs, essential for immune tolerance, was not different than that in control mice, the ratio of CX3CR1intermediate/CX3CR1high proinflammatory/resident macrophages was increased in the colon of CKD mice with higher cytokine expression. Orally administered Lactobacilli mixture partially mitigated CKD-induced “leaky gut,” restored colon epithelial HSP 70, claudin-1, and claudin-2 expression, and decreased apoptosis. Probiotic treatment restored the ratio of CX3CR1intermediate/CX3CR1high macrophages and increased the percentage of CD103+ CD11c+ regulatory dendritic cells, Tregs, in the colon. These changes suppressed systemic inflammation and kidney fibrosis. Our data showed that intestinal dysbiosis-associated gut barrier disruption and aberrant mucosal immunity may be important in the systemic inflammation and progressive fibrosis of CKD. Intestinal targeting may provide novel opportunities for CKD therapy.
목차 (Table of Contents)
- Abstract 7
- I. Introduction 9
- II. Material and methods
- 1. Animal experiments 11
- 2. Analysis of gut bacterial communities 11
- Abstract 7
- I. Introduction 9
- II. Material and methods
- 1. Animal experiments 11
- 2. Analysis of gut bacterial communities 11
- 3. Histological analysis 12
- 4. Intestinal permeability 12
- 5. Western blot analysis 13
- 6. Quantitation of cytokines/chemokines by cytometric bead array 13
- 7. Flow cytometry 13
- 8. Real-time reverse transcriptase PCR 14
- 9. In vitro analysis 14
- 10. Statistical analysis 15
- III. Results
- 1. CKD-induced dysbiosis 16
- 2. Intestinal barrier disruption in CKD is partially mitigated by probiotics 16
- 3. Expansion of proinflammatory macrophages in CKD is partially mitigated by probiotics 17
- 4. Loss of inflammatory anergy of intestinal mononuclear cells in CKD 17
- 5. Probiotics expanded CD4+ Foxp3 Tregs in colon of CKD mice 18
- 6. Probiotics expanded CD11c+ CD103+ regulatory dendritic cells 18
- 7. Effect of probiotics in systemic inflammation and progressive fibrosis in CKD mice 18
- IV. Discussion 20
- Reference 27